
Wearable medical devices are rapidly transforming healthcare, offering individuals unprecedented access to personal health data and enabling proactive health management. From simple fitness trackers to sophisticated diagnostic tools, these devices monitor vital signs, detect anomalies, and provide valuable insights for both individuals and healthcare professionals. This guide explores the various types, accuracy, privacy implications, integration with healthcare systems, and future prospects of this burgeoning field.
We delve into the technological advancements driving this revolution, examining the advantages and disadvantages of different device categories. Crucially, we address the critical aspects of data privacy and security, ensuring informed use and responsible data handling. Finally, we look ahead to the future of wearable medical technology, envisioning how artificial intelligence and machine learning will shape its evolution.
Types of Wearable Medical Devices
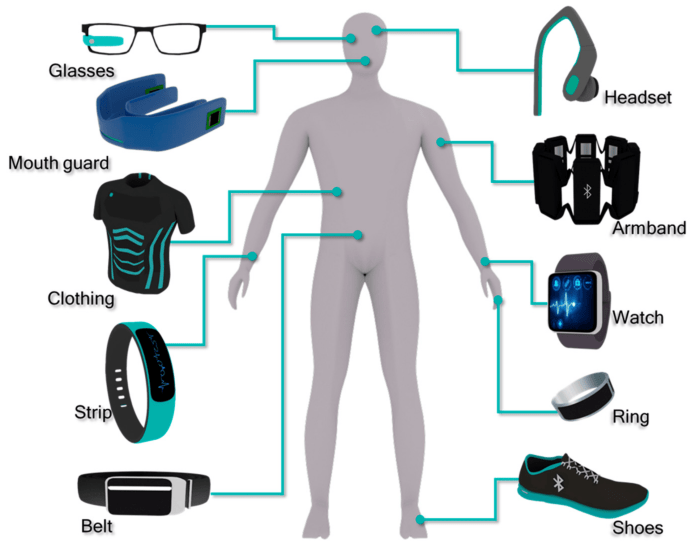
Wearable medical devices represent a rapidly evolving field, offering significant advancements in healthcare monitoring and management. These devices, ranging from simple activity trackers to sophisticated diagnostic tools, empower individuals to take a more active role in their health and enable healthcare professionals to provide more timely and effective interventions. This section will explore the various types of wearable medical devices, their functionalities, and their associated advantages and disadvantages.
Categorization of Wearable Medical Devices by Function and Technology
The following table categorizes wearable medical devices based on their primary function and the underlying technology employed.
| Device Type | Function | Technology | Example |
|---|---|---|---|
| Heart Rate Monitors | Continuous or intermittent measurement of heart rate. | Photoplethysmography (PPG), electrocardiography (ECG) | Smartwatches, fitness trackers |
| Blood Pressure Monitors | Measurement of systolic and diastolic blood pressure. | Oscillometric, mercury sphygmomanometer (less common in wearables) | Wrist-worn blood pressure cuffs, integrated smartwatch sensors (still under development for accurate readings) |
| Sleep Trackers | Monitoring sleep stages, duration, and quality. | Accelerometers, gyroscopes, PPG | Smartwatches, dedicated sleep trackers |
| Glucose Monitors | Continuous or intermittent measurement of glucose levels. | Continuous glucose monitoring (CGM) sensors, electrochemical sensors | CGM patches, integrated smartwatch sensors (limited availability) |
| Electrocardiogram (ECG) Monitors | Detection of heart rhythm irregularities. | Electrodes, signal processing algorithms | Smartwatches, dedicated ECG patches |
| SpO2 Monitors | Measurement of blood oxygen saturation. | Pulse oximetry | Smartwatches, fingertip pulse oximeters (often integrated into smartwatches) |
| Activity Trackers | Monitoring physical activity levels, steps, calories burned. | Accelerometers, gyroscopes | Fitness trackers, smartwatches |
Advantages and Disadvantages of Wearable Medical Devices
Understanding the advantages and disadvantages of each category is crucial for informed decision-making.
Heart Rate Monitors:
- Advantages: Continuous monitoring allows for early detection of heart rate irregularities, improved fitness tracking, and personalized workout optimization.
- Disadvantages: Accuracy can vary depending on the technology used and placement of the device; some individuals may experience skin irritation from sensors.
Blood Pressure Monitors:
- Advantages: Enables regular monitoring of blood pressure, facilitating early detection of hypertension or hypotension.
- Disadvantages: Accuracy can be affected by movement and proper cuff placement; wrist-based monitors may not be as accurate as traditional cuff-based devices.
Sleep Trackers:
- Advantages: Provides insights into sleep patterns, helping individuals identify and address sleep disorders.
- Disadvantages: Accuracy can vary; data may not be clinically validated; reliance on self-reported data can introduce bias.
Glucose Monitors:
- Advantages: Enables continuous monitoring of glucose levels, providing real-time data for better diabetes management.
- Disadvantages: Requires calibration; sensor accuracy can vary; cost can be significant.
ECG Monitors:
- Advantages: Enables early detection of atrial fibrillation and other heart rhythm irregularities.
- Disadvantages: May not detect all types of heart conditions; accuracy depends on proper device placement and signal quality.
Comparison of Smartwatches with ECG Capabilities
This table compares three different smartwatches with ECG capabilities. Note that specific features and accuracy may vary depending on the model and software version.
| Smartwatch | Key Features | ECG Accuracy | Other Notable Features |
|---|---|---|---|
| Apple Watch (Series 8 and later) | ECG app, irregular rhythm notifications, fall detection | Comparable to single-lead ECGs; validated against clinical studies. | Fitness tracking, cellular connectivity, app ecosystem |
| Samsung Galaxy Watch 5 | ECG app, blood pressure monitoring (accuracy limitations), sleep tracking | Generally comparable to other leading smartwatches with ECG. | Fitness tracking, SpO2 monitoring, various watch faces |
| Fitbit Sense | ECG app, EDA sensor (stress tracking), skin temperature sensor | Comparable to other leading smartwatches with ECG. | Fitness tracking, sleep tracking, SpO2 monitoring |
Accuracy and Reliability of Wearable Medical Devices

Wearable medical devices offer convenient and continuous health monitoring, but their accuracy and reliability are crucial considerations. The effectiveness of these devices in providing meaningful health insights hinges on the precision of their readings and the consistency of their performance over time. Factors influencing both accuracy and reliability are complex and multifaceted, requiring careful consideration.The accuracy and reliability of data obtained from wearable medical devices are affected by a variety of factors.
These factors interact in complex ways, making it difficult to isolate the impact of any single element. Understanding these influences is critical for proper interpretation of the data and for making informed healthcare decisions based on this information.
Factors Influencing Accuracy and Reliability
Several factors contribute to the accuracy and reliability of wearable medical device readings. These include the device’s design and technology, the user’s individual characteristics, and environmental conditions. Sensor quality, signal processing algorithms, and data transmission methods all play significant roles. Furthermore, the user’s adherence to instructions, such as proper placement and consistent wear, directly affects data quality. Environmental factors, such as temperature and humidity, can also introduce errors.
For example, a fitness tracker measuring heart rate might be less accurate during strenuous exercise due to movement artifacts, while a smart watch measuring sleep patterns might be affected by ambient light levels.
Potential Sources of Error
Data collected by wearable medical devices is susceptible to various sources of error. These errors can be categorized as systematic or random. Systematic errors are consistent and predictable, often stemming from inherent biases in the device’s design or calibration. Random errors, on the other hand, are unpredictable and vary from one measurement to another. Examples of systematic errors include a consistent overestimation of heart rate due to a faulty sensor, while random errors could be caused by interference from electromagnetic fields or inconsistencies in user placement of the device.
Another important source of error is user-related factors, such as incorrect device usage or failure to follow instructions. For instance, a poorly fitted heart rate monitor can lead to inaccurate readings, and neglecting to properly calibrate a blood pressure monitor can yield unreliable results.
Accuracy Comparison with Established Medical Diagnostic Methods
The accuracy of wearable medical devices varies significantly depending on the specific device and the health metric being measured. A direct comparison against established medical diagnostic methods reveals important nuances.
Below is a comparison of the accuracy of some common wearable medical devices against established medical diagnostic methods:
- Heart Rate Monitoring: Wearable devices generally provide a reasonable estimate of resting heart rate, often within a few beats per minute of an electrocardiogram (ECG). However, during strenuous activity, accuracy can decrease due to motion artifacts. ECG remains the gold standard for precise heart rate measurement.
- Blood Pressure Monitoring: Wearable blood pressure monitors show varying degrees of accuracy compared to traditional sphygmomanometers. While convenient, they may not be as reliable for individuals with irregular heart rhythms or certain medical conditions. Sphygmomanometry remains the established method for accurate blood pressure measurement.
- Sleep Tracking: Wearable sleep trackers provide an approximation of sleep stages (light, deep, REM) and sleep duration. However, their accuracy is limited compared to polysomnography (PSG), the gold standard for sleep studies. PSG involves more extensive monitoring and is usually conducted in a sleep laboratory.
- SpO2 Monitoring: Pulse oximeters integrated into wearables generally provide a good estimate of blood oxygen saturation (SpO2), although accuracy can be affected by factors such as skin pigmentation and motion. Laboratory blood gas analysis remains the definitive method for determining SpO2.
Data Privacy and Security Concerns
The increasing use of wearable medical devices raises significant concerns regarding the privacy and security of sensitive health data. These devices collect a wealth of personal information, often including biometric data, location data, and activity levels, which, if compromised, could have serious consequences for individuals. Understanding these risks and the measures taken to mitigate them is crucial for responsible adoption and usage of this technology.The key risks stem from the vulnerabilities inherent in data collection, transmission, and storage.
Data breaches, unauthorized access, and even accidental data loss can expose sensitive health information, potentially leading to identity theft, discrimination, or misuse of medical information for marketing or other purposes. Furthermore, the lack of standardization in data security protocols across different devices and manufacturers exacerbates these vulnerabilities. The interconnected nature of these devices with smartphones and cloud services also introduces additional points of potential compromise.
Data Security Measures Implemented by Manufacturers
Manufacturers are increasingly recognizing the importance of robust data security and privacy measures. Many employ various techniques to protect user data, including encryption both in transit and at rest. This means that data is scrambled during transmission and storage, making it unreadable without the correct decryption key. They also implement access control measures, limiting access to data based on user roles and permissions.
Regular security audits and penetration testing help identify and address vulnerabilities before they can be exploited. Many companies also adhere to industry standards like HIPAA (Health Insurance Portability and Accountability Act) in the US or GDPR (General Data Protection Regulation) in Europe, demonstrating their commitment to data protection. However, the effectiveness of these measures varies widely depending on the manufacturer and the specific device.
Examples include Fitbit’s commitment to data encryption and its transparency regarding data usage policies, and Apple’s emphasis on end-to-end encryption for health data on its devices.
Hypothetical Privacy Policy for a New Wearable Medical Device
This hypothetical privacy policy Artikels the data collection, usage, and protection practices for “HealthTrack,” a new wearable medical device designed to monitor heart rate, sleep patterns, and activity levels.
Data Collected: HealthTrack collects data such as heart rate, sleep duration and quality, steps taken, distance traveled, and calories burned. It also collects device usage data, such as battery level and connection status. Location data is only collected if explicitly enabled by the user for specific features, such as tracking outdoor workouts. No personally identifiable information (PII) beyond what is necessary for device functionality and user account management is collected.
Data Usage: Collected data is primarily used to provide users with personalized health insights and to improve the accuracy and functionality of the device. Aggregated and anonymized data may be used for research purposes to improve public health understanding, but individual user data will never be shared without explicit consent.
Data Security: HealthTrack employs robust security measures, including data encryption both in transit and at rest, to protect user data from unauthorized access. Access to user data is restricted to authorized personnel only, and regular security audits are conducted to identify and address potential vulnerabilities.
User Rights: Users have the right to access, correct, or delete their data at any time. They can also opt out of data sharing for research purposes and control the types of data collected by the device. HealthTrack is committed to transparent and ethical data handling practices.
Data Retention: User data is retained for as long as the user maintains an active account. Users can request data deletion at any time.
Data Breaches: In the unlikely event of a data breach, HealthTrack will notify affected users as quickly as possible and take appropriate steps to mitigate any potential harm.
The landscape of wearable medical devices is dynamic and promising. While challenges remain regarding data accuracy, privacy, and seamless integration with healthcare systems, the potential benefits are immense. As technology advances and regulatory frameworks evolve, we can expect even more sophisticated devices capable of preventing disease, improving diagnosis, and personalizing treatment. The future of healthcare is undeniably intertwined with the continued innovation and responsible application of wearable medical technology.
Common Queries
What is the average lifespan of a wearable medical device’s battery?
Battery life varies greatly depending on the device and its features. Expect anywhere from a few days to several weeks on a single charge.
Are wearable medical device data compatible across different platforms?
Compatibility varies. Some devices offer seamless integration with multiple platforms (e.g., iOS and Android), while others may be limited to specific ecosystems.
How often should I calibrate my wearable medical device?
Calibration requirements differ per device. Consult your device’s manual for specific instructions. Some devices require no user calibration.
Can I use my wearable medical device while swimming or showering?
Water resistance varies widely. Check the device’s specifications to determine its suitability for use in water.




