Heart disease remains a leading cause of death globally, impacting millions and placing a significant strain on healthcare systems worldwide. Understanding its prevalence, risk factors, and effective treatment strategies is paramount. This exploration delves into the current state of medical research on heart disease, examining advancements in diagnosis, treatment, and prevention, while also highlighting future research directions and the crucial interplay between research, medical services, and device innovation.
From groundbreaking pharmacological interventions to minimally invasive surgical techniques and the development of sophisticated medical devices, the field has witnessed remarkable progress. However, significant challenges remain, including addressing health disparities, improving patient outcomes, and translating research findings into widespread clinical application. This comprehensive overview aims to shed light on these complexities, providing a balanced perspective on the current landscape and future prospects of heart disease research.
Medical Research Advancements in Heart Disease Treatment
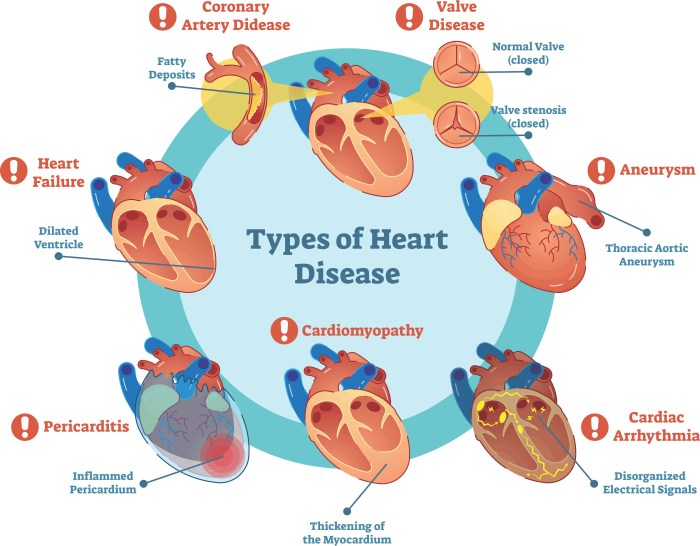
The landscape of heart disease treatment is constantly evolving, driven by ongoing medical research. Significant breakthroughs in pharmacology, minimally invasive surgery, and our understanding of disease mechanisms have led to improved patient outcomes and a higher quality of life for those affected. This section will explore some of the most impactful recent advancements.
Pharmacological advancements have significantly improved the management of heart conditions. New drugs target specific pathways involved in the development and progression of heart disease, offering more precise and effective treatment options with fewer side effects. Minimally invasive surgical techniques have also revolutionized the field, allowing for less traumatic procedures with faster recovery times and reduced risk of complications.
The combination of these advancements has transformed the prognosis for many heart disease patients.
Recent Breakthroughs in Pharmacological Treatment
Recent years have witnessed the development of several novel pharmacological agents that offer improved efficacy and safety profiles compared to older medications. For example, the development of SGLT2 inhibitors has proven revolutionary in the treatment of heart failure, demonstrating a significant reduction in cardiovascular mortality and hospitalization rates. These drugs work by inhibiting the sodium-glucose co-transporter 2, leading to increased sodium and glucose excretion in the urine, ultimately reducing blood pressure and improving cardiac function.
Another example is the emergence of PCSK9 inhibitors, which lower LDL cholesterol levels more effectively than statins alone, benefitting patients with high cholesterol and a high risk of cardiovascular events. These medications work by inhibiting PCSK9, a protein that degrades LDL receptors in the liver, thereby increasing the liver’s capacity to remove LDL cholesterol from the bloodstream.
Mechanisms of Action of Various Heart Medications
Understanding the mechanisms of action of different medications is crucial for effective treatment. Beta-blockers, for instance, reduce heart rate and contractility, lowering blood pressure and myocardial oxygen demand. ACE inhibitors and ARBs block the renin-angiotensin-aldosterone system, reducing blood pressure and vascular remodeling. Statins inhibit cholesterol synthesis, lowering LDL cholesterol levels. Each medication targets specific pathways involved in the development or progression of heart disease, offering a tailored approach to patient management.
Advancements in Minimally Invasive Surgical Procedures
Minimally invasive cardiac surgery has drastically reduced the trauma associated with traditional open-heart surgery. Transcatheter aortic valve replacement (TAVR), for example, allows for the replacement of a diseased aortic valve through a small incision in the groin, minimizing the need for a sternotomy. Similarly, minimally invasive coronary artery bypass grafting (CABG) techniques utilize smaller incisions and specialized instruments, resulting in less pain, shorter hospital stays, and faster recovery times.
These advancements have broadened the treatment options for patients who may not be suitable candidates for traditional open-heart surgery.
Comparison of Treatment Modalities for Heart Conditions
| Heart Condition | Pharmacological Treatment | Surgical Treatment | Other Interventions |
|---|---|---|---|
| Coronary Artery Disease | Statins, Beta-blockers, ACE inhibitors, Aspirin | Coronary artery bypass grafting (CABG), Percutaneous coronary intervention (PCI) | Lifestyle modifications (diet, exercise) |
| Heart Failure | ACE inhibitors, Beta-blockers, Diuretics, SGLT2 inhibitors | Cardiac resynchronization therapy (CRT), Left ventricular assist device (LVAD), Heart transplant | Sodium restriction, fluid management |
Medical Devices Used in Heart Disease Diagnosis and Treatment

The development and application of medical devices have revolutionized the diagnosis and treatment of heart disease, leading to improved patient outcomes and a better understanding of cardiovascular health. These devices range from non-invasive diagnostic tools to sophisticated implantable systems, significantly impacting the field of cardiology. This section will explore the key devices used in both diagnosis and treatment.
Diagnostic Devices in Cardiology
A variety of diagnostic tools provide crucial information about the heart’s structure and function, enabling physicians to accurately assess the presence and severity of heart disease. These devices allow for non-invasive and minimally invasive assessments, improving the speed and accuracy of diagnosis.
- Electrocardiogram (ECG or EKG): An ECG measures the electrical activity of the heart using electrodes placed on the skin. The resulting tracing reveals the heart’s rhythm and can detect abnormalities such as arrhythmias, heart attacks, and electrolyte imbalances. The simplicity and widespread availability of ECGs make it a cornerstone of cardiac diagnosis.
- Echocardiogram: This ultrasound-based imaging technique uses sound waves to create moving pictures of the heart. Echocardiograms provide detailed information about the heart’s chambers, valves, and blood flow, allowing for the detection of structural abnormalities like valve disease, congenital heart defects, and cardiomyopathy. Different echocardiography modalities, such as transthoracic and transesophageal echocardiography, offer varying perspectives and levels of detail.
- Cardiac Catheterization: A more invasive procedure, cardiac catheterization involves inserting a thin, flexible tube (catheter) into a blood vessel and advancing it to the heart. This allows for direct visualization of the coronary arteries, assessment of blood pressure within the heart chambers, and the ability to perform interventions such as angioplasty or stent placement. Cardiac catheterization is crucial for diagnosing coronary artery disease and other structural heart problems.
Implantable Cardiac Devices
Implantable cardiac devices offer long-term management and support for various heart conditions, significantly improving the quality of life for patients with arrhythmias or heart failure. These devices are surgically implanted and provide continuous monitoring and intervention when necessary.
- Pacemakers: Pacemakers are implanted devices that deliver electrical impulses to the heart to regulate its rhythm. They are used to treat bradycardia (slow heart rate) and other rhythm disturbances. Modern pacemakers are sophisticated, offering multiple pacing options and the ability to adjust pacing parameters remotely. For example, a patient with sick sinus syndrome might benefit from a pacemaker to maintain a consistent heart rate.
- Implantable Cardioverter-Defibrillators (ICDs): ICDs are more advanced devices than pacemakers. They monitor the heart’s rhythm and deliver a shock to restore a normal rhythm if a life-threatening arrhythmia, such as ventricular fibrillation, is detected. ICDs are crucial for preventing sudden cardiac death in patients at high risk. A patient with a history of heart attacks and a high ejection fraction might be prescribed an ICD to prevent sudden cardiac death.
Advanced Imaging in Interventional Cardiology
Advanced imaging techniques play a vital role in guiding interventional cardiology procedures, ensuring accuracy and minimizing risks. These techniques provide real-time visualization, allowing cardiologists to precisely navigate catheters and other instruments.
- Intravascular Ultrasound (IVUS): IVUS uses a small ultrasound probe attached to a catheter to provide detailed images of the coronary arteries from within the vessel. This allows for precise assessment of plaque burden, vessel size, and the effectiveness of interventions such as stenting. IVUS is often used during angioplasty to ensure complete stent deployment and to assess the overall condition of the vessel.
- Optical Coherence Tomography (OCT): OCT provides even higher-resolution images of the coronary arteries than IVUS. It uses light waves to create detailed cross-sectional images, allowing for precise assessment of plaque composition and the interaction between the stent and the vessel wall. OCT offers a more detailed visualization than IVUS, allowing for more precise stent placement and improved long-term outcomes.
Impact of Medical Research on Heart Disease Outcomes
Medical research has profoundly reshaped the landscape of heart disease, leading to significant improvements in patient survival rates and quality of life. Decades of dedicated research have yielded groundbreaking advancements, transforming what was once a frequently fatal condition into one that is increasingly manageable and treatable. This impact is evident in both the decreased mortality rates and the enhanced long-term well-being experienced by patients.The introduction of key medical advancements has demonstrably altered the trajectory of heart disease mortality.
For example, the development and widespread adoption of coronary artery bypass grafting (CABG) surgery and percutaneous coronary intervention (PCI), including angioplasty and stenting, have dramatically reduced mortality rates associated with coronary artery disease. Similarly, advancements in the treatment of heart failure, such as the development of ACE inhibitors, beta-blockers, and implantable cardioverter-defibrillators (ICDs), have significantly improved survival and reduced hospitalizations.
Comparing mortality rates from decades past to current statistics reveals a substantial decline, highlighting the success of these interventions.
Heart Disease Mortality Rate Trends
A visual representation of this progress could take the form of a line graph. The x-axis would represent time, spanning several decades, while the y-axis would depict heart disease mortality rates (perhaps expressed as deaths per 100,000 population). The graph would show a clear downward trend, with a relatively steep decline coinciding with the introduction of major medical advancements such as the widespread use of CABG in the 1970s and the increasing adoption of PCI and drug therapies in subsequent decades.
Specific data points could be included to illustrate the impact of these milestones, showcasing a clear correlation between medical breakthroughs and improved survival. The graph would visually demonstrate the substantial reduction in heart disease mortality achieved through ongoing medical research.
Economic Burden and Cost-Effectiveness of Treatment
Heart disease places a considerable economic burden on healthcare systems and individuals worldwide. The costs associated with diagnosis, treatment, hospitalization, and long-term care are substantial. However, many treatment strategies, while expensive upfront, demonstrate cost-effectiveness in the long run by preventing more costly complications such as heart attacks, strokes, and hospital readmissions. For example, while the initial cost of an ICD is high, its preventative effect on sudden cardiac death can lead to significant cost savings in the long term by avoiding expensive emergency care and prolonged hospital stays.
Similarly, the cost of statin therapy, though ongoing, is significantly offset by the reduction in cardiovascular events and their associated costs. Cost-effectiveness analyses are routinely conducted to evaluate the long-term economic implications of various heart disease treatments, guiding healthcare resource allocation.
In conclusion, medical research plays a pivotal role in combating the global burden of heart disease. Continuous advancements in understanding disease mechanisms, developing innovative treatments, and improving diagnostic tools offer hope for improved patient outcomes and reduced mortality rates. Collaboration between researchers, clinicians, and policymakers is essential to overcome remaining challenges and translate promising research into tangible improvements in heart disease care.
The future of heart disease research holds immense potential, with emerging technologies and collaborative efforts paving the way for a healthier future.
Top FAQs
What are the early warning signs of a heart attack?
Chest pain or discomfort, shortness of breath, pain spreading to the arm, jaw, neck, or back, sweating, nausea, lightheadedness. Seek immediate medical attention if you experience these symptoms.
Can heart disease be prevented?
Yes, many risk factors for heart disease are modifiable. Lifestyle changes such as maintaining a healthy weight, regular exercise, a balanced diet, and avoiding smoking significantly reduce the risk.
What is the role of genetics in heart disease?
Genetic predisposition plays a role, but lifestyle factors often have a greater impact. Family history increases risk, but healthy choices can mitigate this.
How often should I have a heart health checkup?
Frequency depends on age, risk factors, and family history. Consult your doctor to determine the appropriate schedule for your individual needs.




